The “Invisible” Kick That Ruins Your 8 Hours: Understanding PLMD & RLS
If your legs feel electric at bedtime or your partner notices rhythmic kicking during sleep, you are not imagining it. Periodic Limb Movement Disorder (PLMD) and Restless Legs Syndrome (RLS) are medically real patterns with measurable mechanisms. The good news is that once we separate symptom type, test ferritin correctly, and rebuild evening triggers, sleep quality can improve within weeks for many people.
- RLS usually disrupts sleep onset while awake; PLMD fragments sleep after sleep begins.
- Ferritin targets for sleep are often higher than standard “not-anemic” lab thresholds.
- Trigger control plus a practical night protocol works better than random supplements.

1) Science Behind RLS & PLMD: What Is Happening in the Brain and Body
Sleep disruption is rarely one-dimensional. Body exhaustion does not guarantee sleep onset—a critical distinction often missed. RLS patients frequently experience a paradox: they feel deeply tired physically, yet their legs remain neurologically overactivated, preventing the transition to sleep. Furthermore, creeping, tingling, or electric sensations are not merely “stress” or “anxiety”; they are physiological signals that require proper medical screening rather than dismissal.
From a mechanism standpoint, RLS is strongly associated with dopaminergic signaling dysregulation and low brain-available iron. PLMD is different: repetitive limb movements occur during sleep cycles and produce micro-arousals that reduce restorative continuity. Many people wake up saying “I slept enough hours but still feel wrecked” because quantity survived while architecture collapsed.
Major clinical reviews and sleep-medicine practice patterns consistently show that ferritin interpretation for sleep complaints is often stricter than general anemia screening. In routine practice, some sleep specialists target ferritin above 50-75 ng/mL before symptom improvement stabilizes. This does not replace physician care, but it explains why “normal CBC” can coexist with persistent night symptoms.
Our evidence lens also aligns with the authority voices we cite across Slumbelry’s framework: Matthew Walker on architecture integrity, Dr. Neil Stanley on fragile sleep continuity, and Dr. Robert Rosenberg on hidden medical disruptors including RLS and PLMD patterns. The practical takeaway is simple: when the nervous system is repeatedly interrupted, deeper N3 and REM opportunities shrink, even if your clock says you were in bed for seven or eight hours. That is why this topic belongs in medical-grade sleep conversations, not in the “just relax” bucket.
| Dimension | RLS | PLMD |
|---|---|---|
| Primary timing | Before sleep, while awake | After sleep onset, during sleep |
| Main experience | Urge to move, crawling/electric discomfort | Rhythmic kicks or twitches every ~20-40 seconds |
| Main damage | Delayed sleep onset | Sleep fragmentation and micro-arousals |
| Core first checks | Ferritin, trigger drugs, evening stimulants | Sleep study context, partner reports, architecture disruption |
Science gently suggests this: if symptoms are repetitive, time-linked, and movement-relieved, we should stop blaming personality and start rebuilding physiology.
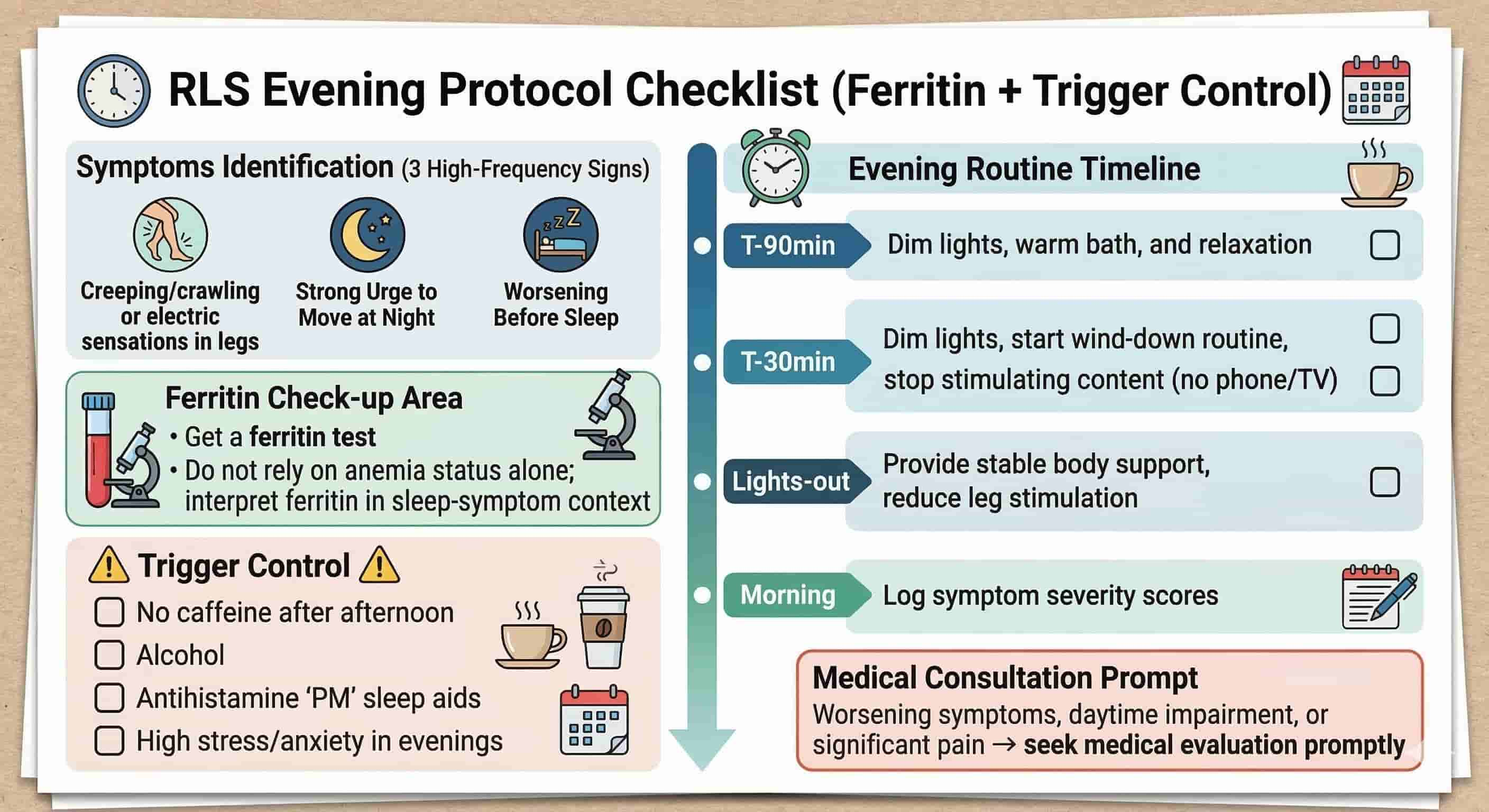
2) Practical Protocol: 5 Steps to Calm Night Legs and Protect Sleep Architecture
We do this together, one stable step at a time. This protocol is educational and should be coordinated with your clinician when medication, pregnancy, chronic disease, or severe daytime impairment is present.
- Within 7 days, run the right lab conversation. Ask for ferritin-focused interpretation for sleep symptoms, not only anemia status. Bring your symptom log: onset time, leg sensation intensity, movement relief latency, and next-day fatigue score.
- For 14 nights, remove known amplifiers after 2 PM. Cut caffeine and limit alcohol; review antihistamine-heavy “PM” products with your doctor. If you need help with stimulant timing, see The Caffeine Curfew.
- At T-90 minutes before bed, start a downshift block. Warm shower, gentle calf release, low light, no doom-scrolling. Pair this with Circadian Reset protocol logic so your nervous system receives one clear signal: night equals safety.
- At lights-out, reduce mechanical irritation. Use stable spinal support and pressure-balanced bedding. For sensory-sensitive sleepers, a structured support pillow can reduce compensatory tossing; reference Butterfly Pillow and your broader sleep environment setup in Sleep Sanctuary.
- Each morning, score outcomes in under 2 minutes. Sleep onset delay, night awakenings, partner movement observations, morning refresh score. Then run our Sleep Assessment weekly to detect trend direction, not just one bad night.
Clinical stability tip: if daytime sleepiness, mood decline, or leg pain escalates despite protocol adherence, escalate to formal sleep medicine review rather than stacking random supplements.
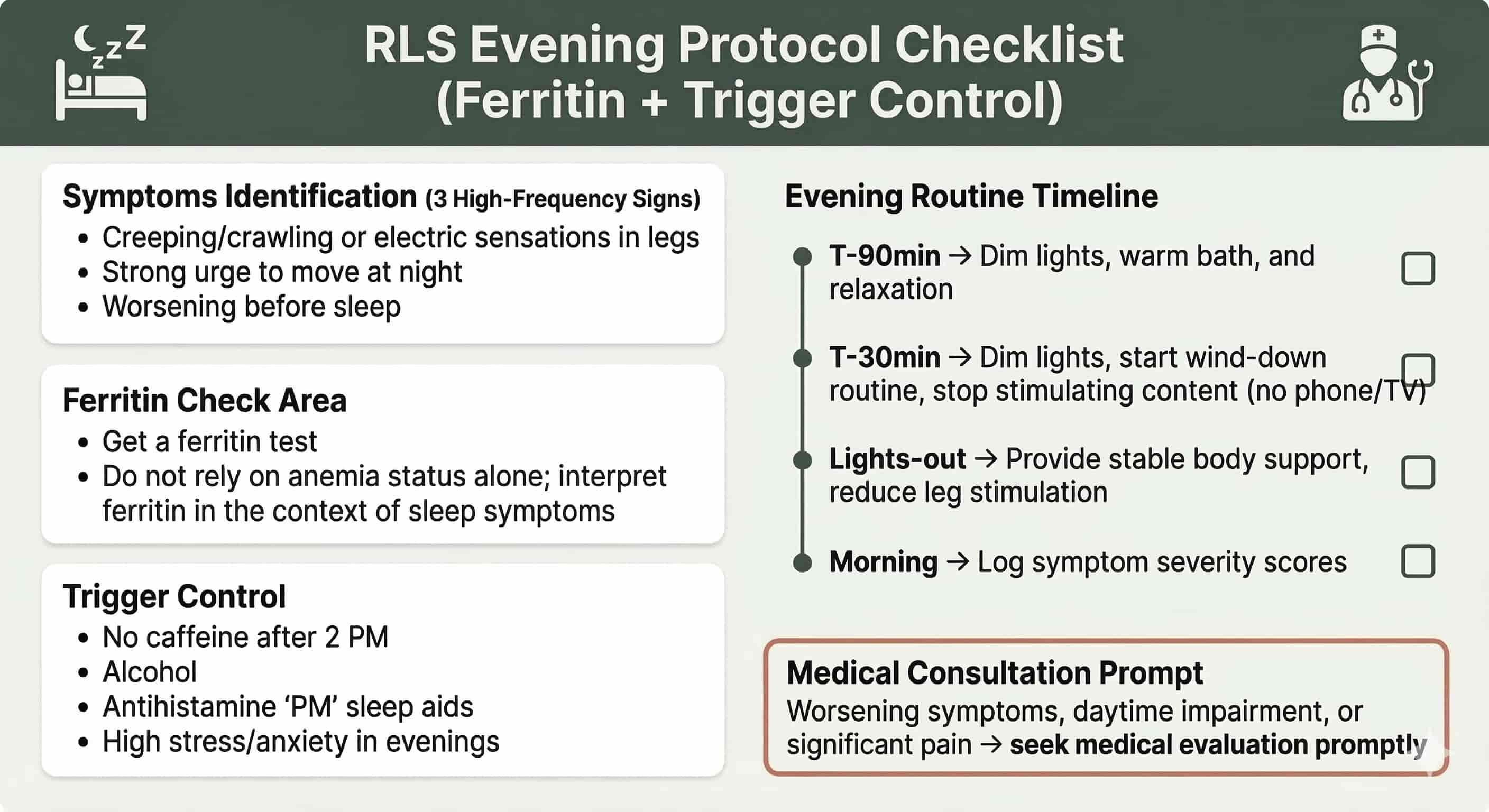
3) Common Mistakes and FAQ
Q1: If my hemoglobin is normal, can iron still be relevant for sleep?
Yes. General blood normality does not automatically mean optimal iron availability for RLS-related sleep symptoms. Ferritin context matters and should be interpreted with sleep-specific complaints in mind.
Q2: Is this just anxiety, not a real disorder?
No. Anxiety can amplify symptom perception, but RLS/PLMD has recognized neurological and sleep-architecture signatures. It is both mind-and-body, not imaginary.
Q3: Should I self-medicate first or test first?
Test first whenever possible. Starting supplements or sedatives blindly can mask drivers and delay proper treatment. Begin with targeted data, then iterate.
4) What to Do Tonight: Gentle, Structured, Forward
You do not need a perfect night to start winning. You need a repeatable system. Tonight, choose one measurable action: start your T-90 routine, log symptom timing, and remove one trigger. Over 2-3 weeks, trend beats panic.
If you want a personalized next step, begin with our Sleep Assessment workflow, then subscribe to our newsletter for weekly protocol updates and case-based guidance built around the Slumbelry Sleep System.
Stop letting your nervous system hijack your nights. Start taking control of your biological sleep drive today.
Take the Free Sleep Assessment Join the Recovery NewsletterThe Slumbelry Commitment
Sleep is the most vulnerable state of human existence. It is where we heal, reset, and grow.
At Slumbelry, we don’t just sell sleep products; we advocate for your physiological right to rest. From ergonomic support to light management, every solution we offer is designed with one obsession: Respecting your Biology.
Science is our language, but your recovery is our purpose. You take care of everything else in your life—let us take care of your nights.
Rest Deeply,
The Slumbelry Team
Slumbelry™ Sleep System – Science-Backed. Chronotype-Optimized. Author: Slumbelry Research Team.
